Purpose of This Guideline
Date of current publication: November 22, 2024
Lead author: Shauna Gunaratne, MD, MPH, DTM&H
Writing group: Rona M. Vail, MD, AAHIVS; Sanjiv S. Shah, MD, MPH, AAHIVS; Steven M. Fine, MD, PhD; Joseph P. McGowan, MD, FACP, FIDSA, AAHIVS; Samuel T. Merrick, MD, FIDSA; Asa E. Radix, MD, MPH, PhD, FACP, AAHIVS; Anne K. Monroe, MD, MSPH; Jessica Rodrigues, MPH, MS; Christopher J. Hoffmann, MD, MPH, MSc, FACP; Brianna L. Norton, DO, MPH; Charles J. Gonzalez, MD
Committee: Medical Care Criteria Committee
Date of original publication: September 10, 2019
This guideline was developed by the New York State Department of Health (NYSDOH) AIDS Institute (AI) to establish an evidence-based approach to routine laboratory monitoring of antiretroviral toxicity. Data are lacking regarding the need for and frequency of routine laboratory monitoring in patients taking oral and long-acting injectable antiretroviral therapy (ART). To date, no randomized controlled studies have assessed the optimal type and frequency of monitoring. The data available are based on short-term randomized clinical trials of ART strategies, observational cohort data, and long-term epidemiologic data.
The guideline aims to achieve the following goals:
- Assist clinicians in determining the frequency of routine laboratory monitoring for adverse effects of ART.
- Inform clinicians about the range of adverse effects and toxicities associated with ART.
Refer to the NYSDOH AI guideline Primary Care for Adults With HIV for information on other routine laboratory monitoring for patients with HIV.
Frequency of Laboratory Monitoring During ART
| RECOMMENDATION |
Frequency of Laboratory Monitoring During ART
|
Note:
|
This guideline summarizes the recommended minimum frequency of routine laboratory monitoring in healthy patients receiving ART. Patients with HIV should also be monitored for relevant age- and sex-specific health problems Thompson, et al. 2021. Patients with comorbidities, or who take or start additional medications, or who have baseline laboratory abnormalities may require more frequent or additional evaluation. NYSDOH AI recommendations apply to resource-rich settings; World Health Organization guidelines do not require access to laboratory monitoring as a condition for initiation or continuation of ART.
This committee’s recommendations diverge from those of other published guidelines in that they suggest less frequent monitoring for ART-related adverse effects UpToDate 2023; DHHS 2022. The reduced frequency of testing reflects the notably reduced toxicities associated with contemporary antiretroviral regimens, earlier initiation of ART, and the absence of data to support more frequent testing. This guideline also suggests less frequent monitoring after the first year of ART or at regimen change, based on the observation that most laboratory-detected toxicities occur in the first year of therapy Gudina, et al. 2017. This guideline applies to both oral and long-acting injectable formulations of ART.
The guideline section Screening for Organ-Specific Adverse Effects discusses the range of adverse effects and toxicities associated with ART. Patients rarely present with symptoms suggestive of antiretroviral toxicity; frequent laboratory monitoring may be needed in such cases.
| Abbreviations: ALT, alanine aminotransferase; ART, antiretroviral therapy; AST, aspartate aminotransferase; eGFR, estimated glomerular filtration rate; INSTI, integrase strand transfer inhibitor; PI, protease inhibitor; TAF, tenofovir alafenamide; TDF, tenofovir disoproxil fumarate; ZDV, zidovudine.
Notes:
|
|||||
| Table 1: Minimum Laboratory Monitoring Frequency With Initiation of or Change in Oral and Long-Acting Injectable ART for Patients Aged <50 Years and Without Chronic Comorbidities [a] (Rating: A3) | |||||
| Laboratory Tests | Year 1 of ART (initiation or change) | After 1 Year on ART Regimen | |||
| Baseline | 3 Months [b] | 12 Months | Every 6 Months | Annual | |
| Hepatic panel (AST, ALT, alkaline phosphatase, total bilirubin) | All | All | All | — | All |
| Random blood glucose | All | All | All | — | With INSTIs or PIs |
| Complete blood count [c] | All | With ZDV | With ZDV | With ZDV | — |
| eGFR [d] | All | All | With TAF or TDF | — | With TAF or TDF [a] |
| Test for proteinuria (urinalysis or protein-to-creatinine ratio), glucosuria, serum phosphorus | With TAF or TDF | — | With TAF or TDF | — | With TAF or TDF |
Screening for Organ-Specific Adverse Effects
Nephrotoxicity: Antiretroviral therapy (ART) has been associated with a range of renal complications that may lead to renal insufficiency or failure Hall, et al. 2011. Furthermore, renal impairment requires dose adjustment or discontinuation of several antiretroviral agents (ARVs). Various guidelines recommend screening for ART-induced nephrotoxicity DHHS 2024; Cervantes and Atta 2023; Gillis, et al. 2015. Data to support screening strategies and frequency are most robust for the detection of ART-associated kidney dysfunction than other organ-specific toxicities. Nevertheless, many recommendations continue to rely on expert opinion and consensus. Patients with reduced baseline renal function and those taking concomitant nephrotoxic medications may require more frequent renal monitoring, as clinically indicated.
A number of ARVs have been implicated in kidney dysfunction. However, only medications that contain tenofovir prodrugs are considered directly nephrotoxic to the renal tubules and glomeruli. Tenofovir disoproxil fumarate (TDF) and tenofovir alafenamide (TAF) are both prodrugs of tenofovir and are widely used components of antiretroviral regimens in the United States. Because various forms of renal impairment have been reported in patients receiving tenofovir prodrugs Cervantes and Atta 2023, specific recommendations regarding frequency of laboratory monitoring for regimens that include these agents have been made in Table 1: Minimum Laboratory Monitoring Frequency With Initiation of or Change in ART for Patients Aged <50 Years and Without Chronic Comorbidities.
Plasma concentrations of tenofovir are approximately 4-fold lower with use of TAF than with TDF, and while nephrotoxicity due to TAF is rare, cases of acute renal failure, proximal renal tubulopathy, and possible Fanconi Syndrome have been reported in clinical use Bahr and Yarlagadda 2019; Novick, et al. 2017. Therefore, Table 1 provides recommendations for frequency of monitoring of renal function in patients taking tenofovir prodrugs (TDF and TAF) that does not distinguish formulation used.
Either of the MDRD or CKD-EPI equations can be used to measure estimated glomerular filtration rates (GFRs, see the National Institute of Diabetes and Digestive and Kidney Diseases Health Information Center Glomerular Filtration Rate Calculators). Using the same method of estimation over time is recommended. Certain ARVs have been associated with decreased glomerular secretion of creatinine, leading to a small rise in serum creatinine levels without concomitant decline in GFR. These agents include rilpivirine, dolutegravir, bictegravir, and the pharmaco-enhancer cobicistat. A consensus statement from Australia recommends that serum creatinine levels be checked 1 month after initiation of these agents to establish a new “baseline” measurement Holt, et al. 2014. Estimation of GFR with a serum cystatin C measurement may provide a more accurate assessment in patients taking agents that affect creatinine secretion and is increasingly utilized in clinical practice Galizzi, et al. 2018; Yukawa, et al. 2018.
Finally, a number of protease inhibitors (PIs), including atazanavir, have been shown to cause crystal-induced nephropathy.
| KEY POINT |
|
Hepatotoxicity: Most ARVs have the potential to cause idiopathic abnormalities in liver function, especially in patients with preexisting liver disease. As a class, non-nucleoside reverse transcriptase inhibitors (NNRTIs) show the highest rates of hepatotoxicity, most notably with the first-generation NNRTI nevirapine and, to a lesser extent, efavirenz. Because drug-induced hepatotoxicity of any kind generally occurs within the first 6 to 12 weeks of treatment, there is no recommended distinction in terms of frequency of monitoring based on the ART regimen. Current evidence does not show associations between specific ARTs and abnormal liver enzymes in patients on long-term ART Chew, et al. 2023.
Dyslipidemia, insulin resistance, and diabetes mellitus: ART has been associated with weight gain, dyslipidemia, metabolic syndrome, insulin resistance, and new-onset diabetes mellitus (see NYSDOH AI guideline Primary Care for Adults With HIV > HIV-Specific Primary Care > Metabolic changes). A range of untoward lipid effects has been observed with a variety of ARVs, including PIs, NNRTIs, and certain nucleoside reverse transcriptase inhibitors (NRTIs) Kalra, et al. 2023. In general, such changes are small and do not result in pharmacologic changes to lipid management.
Emerging evidence has shown weight gain associated with switching from TDF to TAF and switching from NNRTI-based regimens to integrase strand transfer inhibitor (INSTI)-based regimens, especially when the switches occur together Erlandson, et al. 2021; Mallon, et al. 2021; Surial, et al. 2021; van Wyk, et al. 2021; Bourgi, et al. 2020; Lake, et al. 2020; Venter, et al. 2020. The observed effect of weight gain may be due to cessation of weight suppression caused by TDF and, possibly, NNRTI-based regimens. This information may help care providers more accurately frame the discussion with patients on observed weight gain with ARV switches Bosch, et al. 2023; Bourgi, et al. 2023.
The traditional risk factors for metabolic disorders—such as age, weight, and diet—are stronger risk factors for metabolic disease than ART toxicity. Nevertheless, in several studies, patients with HIV had a higher rate of cardiovascular disease than controls without HIV Hirsch, et al. 2024; Grinspoon, et al. 2023; Freiberg, et al. 2013; Currier, et al. 2003 (see 2023 AHA/ACC/ACCP/ASPC/NLA/PCNA Guideline for the Management of Patients With Chronic Coronary Disease). The use of certain ritonavir-boosted PIs has been associated with an increased risk of myocardial infarction in long-term observational studies Ryom, et al. 2018; Friis-Moller, et al. 2007. Current or prior abacavir use has also been associated with an elevated risk of cardiovascular events and myocardial infarction in persons with HIV, as seen in multiple large cohort studies Fichtenbaum, et al. 2024; Jaschinski, et al. 2023; Elion, et al. 2018. INSTI-based regimens have been associated with a higher risk of development of diabetes mellitus than non-INSTI-based regimens [O’Halloran, et al. 2022; Rebeiro, et al. 2021].
Table 1: Minimum Laboratory Monitoring Frequency With Initiation of or Change in ART for Patients Aged <50 Years and Without Chronic Comorbidities does not provide specific recommendations for lipid profile testing in patients on ART. In most patients, screening should follow recommendations for patients without HIV Avgousti and Feinstein 2023; Grinspoon, et al. 2023; Feinstein, et al. 2019. However, clinicians may opt to perform more frequent lipid testing in patients with underlying cardiovascular comorbidities and those taking a PI-based therapy. Clinicians may also opt to perform diabetes mellitus screening in patients with weight gain after initiating ART and those on INSTI-based regimens.
Cytopenias: Bone marrow suppression as a consequence of ART is rare and most often associated with the use of zidovudine. The most common cytopenia caused by zidovudine is a macrocytic anemia. In resource-rich settings, early treatment and newer regimens have made cytopenias an extremely rare complication of ART. Only patients receiving zidovudine as part of their antiretroviral regimen require monitoring of blood counts.
Pancreatitis and lactic acidosis: In the early era of ART, the NRTIs stavudine and didanosine were associated with a significantly increased risk of both pancreatitis and lactic acidosis. However, pancreatitis and lactic acidosis are exceedingly rare complications with current ART regimens. Therefore, routine laboratory monitoring of serum lipase and lactic acid to detect these abnormalities is not recommended with contemporary ART regimens.
All Recommendations
| ALL RECOMMENDATIONS: LABORATORY MONITORING FOR ADVERSE EFFECTS OF ART |
Frequency of Laboratory Monitoring During ART
|
Note:
|
Shared Decision-Making
Download Printable PDF of Shared Decision-Making Statement
Date of current publication: August 8, 2023
Lead authors: Jessica Rodrigues, MS; Jessica M. Atrio, MD, MSc; and Johanna L. Gribble, MA
Writing group: Steven M. Fine, MD, PhD; Rona M. Vail, MD; Samuel T. Merrick, MD; Asa E. Radix, MD, MPH, PhD; Christopher J. Hoffmann, MD, MPH; Charles J. Gonzalez, MD
Committee: Medical Care Criteria Committee
Date of original publication: August 8, 2023
Rationale
Throughout its guidelines, the New York State Department of Health (NYSDOH) AIDS Institute (AI) Clinical Guidelines Program recommends “shared decision-making,” an individualized process central to patient-centered care. With shared decision-making, clinicians and patients engage in meaningful dialogue to arrive at an informed, collaborative decision about a patient’s health, care, and treatment planning. The approach to shared decision-making described here applies to recommendations included in all program guidelines. The included elements are drawn from a comprehensive review of multiple sources and similar attempts to define shared decision-making, including the Institute of Medicine’s original description [Institute of Medicine 2001]. For more information, a variety of informative resources and suggested readings are included at the end of the discussion.
Benefits
The benefits to patients that have been associated with a shared decision-making approach include:
- Decreased anxiety [Niburski, et al. 2020; Stalnikowicz and Brezis 2020]
- Increased trust in clinicians [Acree, et al. 2020; Groot, et al. 2020; Stalnikowicz and Brezis 2020]
- Improved engagement in preventive care [McNulty, et al. 2022; Scalia, et al. 2022; Bertakis and Azari 2011]
- Improved treatment adherence, clinical outcomes, and satisfaction with care [Crawford, et al. 2021; Bertakis and Azari 2011; Robinson, et al. 2008]
- Increased knowledge, confidence, empowerment, and self-efficacy [Chen, et al. 2021; Coronado-Vázquez, et al. 2020; Niburski, et al. 2020]
Approach
Collaborative care: Shared decision-making is an approach to healthcare delivery that respects a patient’s autonomy in responding to a clinician’s recommendations and facilitates dynamic, personalized, and collaborative care. Through this process, a clinician engages a patient in an open and respectful dialogue to elicit the patient’s knowledge, experience, healthcare goals, daily routine, lifestyle, support system, cultural and personal identity, and attitudes toward behavior, treatment, and risk. With this information and the clinician’s clinical expertise, the patient and clinician can collaborate to identify, evaluate, and choose from among available healthcare options [Coulter and Collins 2011]. This process emphasizes the importance of a patient’s values, preferences, needs, social context, and lived experience in evaluating the known benefits, risks, and limitations of a clinician’s recommendations for screening, prevention, treatment, and follow-up. As a result, shared decision-making also respects a patient’s autonomy, agency, and capacity in defining and managing their healthcare goals. Building a clinician-patient relationship rooted in shared decision-making can help clinicians engage in productive discussions with patients whose decisions may not align with optimal health outcomes. Fostering open and honest dialogue to understand a patient’s motivations while suspending judgment to reduce harm and explore alternatives is particularly vital when a patient chooses to engage in practices that may exacerbate or complicate health conditions [Halperin, et al. 2007].
Options: Implicit in the shared decision-making process is the recognition that the “right” healthcare decisions are those made by informed patients and clinicians working toward patient-centered and defined healthcare goals. When multiple options are available, shared decision-making encourages thoughtful discussion of the potential benefits and potential harms of all options, which may include doing nothing or waiting. This approach also acknowledges that efficacy may not be the most important factor in a patient’s preferences and choices [Sewell, et al. 2021].
Clinician awareness: The collaborative process of shared decision-making is enhanced by a clinician’s ability to demonstrate empathic interest in the patient, avoid stigmatizing language, employ cultural humility, recognize systemic barriers to equitable outcomes, and practice strategies of self-awareness and mitigation against implicit personal biases [Parish, et al. 2019].
Caveats: It is important for clinicians to recognize and be sensitive to the inherent power and influence they maintain throughout their interactions with patients. A clinician’s identity and community affiliations may influence their ability to navigate the shared decision-making process and develop a therapeutic alliance with the patient and may affect the treatment plan [KFF 2023; Greenwood, et al. 2020]. Furthermore, institutional policy and regional legislation, such as requirements for parental consent for gender-affirming care for transgender people or insurance coverage for sexual health care, may infringe upon a patient’s ability to access preventive- or treatment-related care [Sewell, et al. 2021].
Figure 1: Elements of Shared Decision-Making
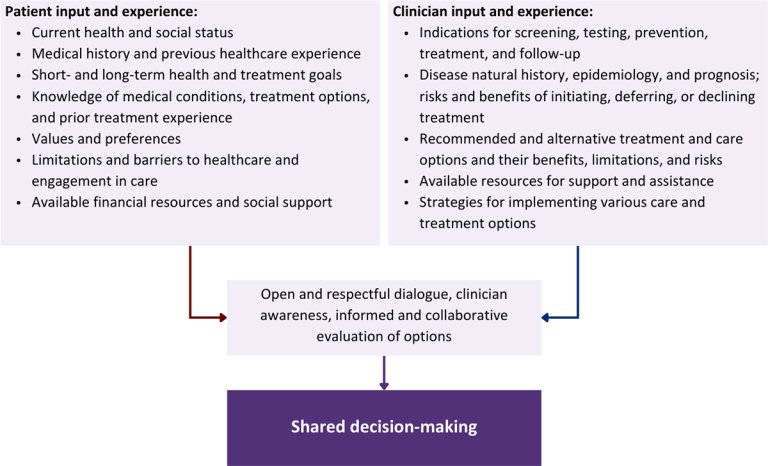
Health equity: Adapting a shared decision-making approach that supports diverse populations is necessary to achieve more equitable and inclusive health outcomes [Castaneda-Guarderas, et al. 2016]. For instance, clinicians may need to incorporate cultural- and community-specific considerations into discussions with women, gender-diverse individuals, and young people concerning their sexual behaviors, fertility intentions, and pregnancy or lactation status. Shared decision-making offers an opportunity to build trust among marginalized and disenfranchised communities by validating their symptoms, values, and lived experience. Furthermore, it can allow for improved consistency in patient screening and assessment of prevention options and treatment plans, which can reduce the influence of social constructs and implicit bias [Castaneda-Guarderas, et al. 2016].
Clinician bias has been associated with health disparities and can have profoundly negative effects [FitzGerald and Hurst 2017; Hall, et al. 2015]. It is often challenging for clinicians to recognize and set aside personal biases and to address biases with peers and colleagues. Consciously or unconsciously, negative or stigmatizing assumptions are often made about patient characteristics, such as race, ethnicity, gender, sexual orientation, mental health, and substance use [Avery, et al. 2019; van Boekel, et al. 2013; Livingston, et al. 2012]. With its emphasis on eliciting patient information, a shared decision-making approach encourages clinicians to inquire about patients’ lived experiences rather than making assumptions and to recognize the influence of that experience in healthcare decision-making.
Stigma: Stigma may prevent individuals from seeking or receiving treatment and harm reduction services [Tsai, et al. 2019]. Among people with HIV, stigma and medical mistrust remain significant barriers to healthcare utilization, HIV diagnosis, and medication adherence and can affect disease outcomes [Turan, et al. 2017; Chambers, et al. 2015], and stigma among clinicians against people who use substances has been well-documented [Stone, et al. 2021; Tsai, et al. 2019; van Boekel, et al. 2013]. Sexual and reproductive health, including strategies to prevent HIV transmission, acquisition, and progression, may be subject to stigma, bias, social influence, and violence.
| SHARED DECISION-MAKING IN HIV CARE |
|
Resources and Suggested Reading
In addition to the references cited below, the following resources and suggested reading may be useful to clinicians.
| RESOURCES |
References
Acree ME, McNulty M, Blocker O, et al. Shared decision-making around anal cancer screening among black bisexual and gay men in the USA. Cult Health Sex 2020;22(2):201-16. [PMID: 30931831]
Avery JD, Taylor KE, Kast KA, et al. Attitudes toward individuals with mental illness and substance use disorders among resident physicians. Prim Care Companion CNS Disord 2019;21(1):18m02382. [PMID: 30620451]
Bertakis KD, Azari R. Patient-centered care is associated with decreased health care utilization. J Am Board Fam Med 2011;24(3):229-39. [PMID: 21551394]
Castaneda-Guarderas A, Glassberg J, Grudzen CR, et al. Shared decision making with vulnerable populations in the emergency department. Acad Emerg Med 2016;23(12):1410-16. [PMID: 27860022]
Chambers LA, Rueda S, Baker DN, et al. Stigma, HIV and health: a qualitative synthesis. BMC Public Health 2015;15:848. [PMID: 26334626]
Chen CH, Kang YN, Chiu PY, et al. Effectiveness of shared decision-making intervention in patients with lumbar degenerative diseases: a randomized controlled trial. Patient Educ Couns 2021;104(10):2498-2504. [PMID: 33741234]
Coronado-Vázquez V, Canet-Fajas C, Delgado-Marroquín MT, et al. Interventions to facilitate shared decision-making using decision aids with patients in primary health care: a systematic review. Medicine (Baltimore) 2020;99(32):e21389. [PMID: 32769870]
Coulter A, Collins A. Making shared decision-making a reality: no decision about me, without me. 2011. https://www.kingsfund.org.uk/sites/default/files/Making-shared-decision-making-a-reality-paper-Angela-Coulter-Alf-Collins-July-2011_0.pdf
Crawford J, Petrie K, Harvey SB. Shared decision-making and the implementation of treatment recommendations for depression. Patient Educ Couns 2021;104(8):2119-21. [PMID: 33563500]
FitzGerald C, Hurst S. Implicit bias in healthcare professionals: a systematic review. BMC Med Ethics 2017;18(1):19. [PMID: 28249596]
Greenwood BN, Hardeman RR, Huang L, et al. Physician-patient racial concordance and disparities in birthing mortality for newborns. Proc Natl Acad Sci U S A 2020;117(35):21194-21200. [PMID: 32817561]
Groot G, Waldron T, Barreno L, et al. Trust and world view in shared decision making with indigenous patients: a realist synthesis. J Eval Clin Pract 2020;26(2):503-14. [PMID: 31750600]
Hall WJ, Chapman MV, Lee KM, et al. Implicit racial/ethnic bias among health care professionals and its influence on health care outcomes: a systematic review. Am J Public Health 2015;105(12):e60-76. [PMID: 26469668]
Halperin B, Melnychuk R, Downie J, et al. When is it permissible to dismiss a family who refuses vaccines? Legal, ethical and public health perspectives. Paediatr Child Health 2007;12(10):843-45. [PMID: 19043497]
Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. 2001. https://www.ncbi.nlm.nih.gov/books/NBK222274/
KFF. Key data on health and health care by race and ethnicity. 2023 Mar 15. https://www.kff.org/racial-equity-and-health-policy/report/key-data-on-health-and-health-care-by-race-and-ethnicity/ [accessed 2023 May 19]
Livingston JD, Milne T, Fang ML, et al. The effectiveness of interventions for reducing stigma related to substance use disorders: a systematic review. Addiction 2012;107(1):39-50. [PMID: 21815959]
McNulty MC, Acree ME, Kerman J, et al. Shared decision making for HIV pre-exposure prophylaxis (PrEP) with black transgender women. Cult Health Sex 2022;24(8):1033-46. [PMID: 33983866]
Niburski K, Guadagno E, Abbasgholizadeh-Rahimi S, et al. Shared decision making in surgery: a meta-analysis of existing literature. Patient 2020;13(6):667-81. [PMID: 32880820]
Parish SJ, Hahn SR, Goldstein SW, et al. The International Society for the Study of Women’s Sexual Health process of care for the identification of sexual concerns and problems in women. Mayo Clin Proc 2019;94(5):842-56. [PMID: 30954288]
Robinson JH, Callister LC, Berry JA, et al. Patient-centered care and adherence: definitions and applications to improve outcomes. J Am Acad Nurse Pract 2008;20(12):600-607. [PMID: 19120591]
Scalia P, Durand MA, Elwyn G. Shared decision-making interventions: an overview and a meta-analysis of their impact on vaccine uptake. J Intern Med 2022;291(4):408-25. [PMID: 34700363]
Sewell WC, Solleveld P, Seidman D, et al. Patient-led decision-making for HIV preexposure prophylaxis. Curr HIV/AIDS Rep 2021;18(1):48-56. [PMID: 33417201]
Stalnikowicz R, Brezis M. Meaningful shared decision-making: complex process demanding cognitive and emotional skills. J Eval Clin Pract 2020;26(2):431-38. [PMID: 31989727]
Stone EM, Kennedy-Hendricks A, Barry CL, et al. The role of stigma in U.S. primary care physicians’ treatment of opioid use disorder. Drug Alcohol Depend 2021;221:108627. [PMID: 33621805]
Tsai AC, Kiang MV, Barnett ML, et al. Stigma as a fundamental hindrance to the United States opioid overdose crisis response. PLoS Med 2019;16(11):e1002969. [PMID: 31770387]
Turan B, Budhwani H, Fazeli PL, et al. How does stigma affect people living with HIV? The mediating roles of internalized and anticipated HIV stigma in the effects of perceived community stigma on health and psychosocial outcomes. AIDS Behav 2017;21(1):283-91. [PMID: 27272742]
van Boekel LC, Brouwers EP, van Weeghel J, et al. Stigma among health professionals towards patients with substance use disorders and its consequences for healthcare delivery: systematic review. Drug Alcohol Depend 2013;131(1-2):23-35. [PMID: 23490450]
References
Avgousti H., Feinstein M. J. Prevention and treatment of cardiovascular disease in HIV: practical insights in an evolving field. Top Antivir Med 2023;31(5):559-65. [PMID: 38198667]
Bahr N. C., Yarlagadda S. G. Fanconi syndrome and tenofovir alafenamide: a case report. Ann Intern Med 2019;170(11):814-15. [PMID: 30690644]
Bosch B., Akpomiemie G., Chandiwana N., et al. Weight and metabolic changes after switching from tenofovir alafenamide/emtricitabine (FTC)+dolutegravir (DTG), tenofovir disoproxil fumarate (TDF)/FTC + DTG, and TDF/FTC/efavirenz to TDF/lamivudine/DTG. Clin Infect Dis 2023;76(8):1492-95. [PMID: 36519389]
Bourgi K., Jenkins C. A., Rebeiro P. F., et al. Weight gain among treatment-naïve persons with HIV starting integrase inhibitors compared to non-nucleoside reverse transcriptase inhibitors or protease inhibitors in a large observational cohort in the United States and Canada. J Int AIDS Soc 2020;23(4):e25484. [PMID: 32294337]
Bourgi K., Ofner S., Musick B., et al. Preswitch regimens influence the rate of weight gain after switch to tenofovir disoproxil fumarate, lamivudine, and dolutegravir (TLD): study from an East African cohort. Open Forum Infect Dis 2023;10(12):ofad581. [PMID: 38088979]
Cervantes C. E., Atta M. G. Updates on HIV and kidney disease. Curr HIV/AIDS Rep 2023;20(2):100-110. [PMID: 36695948]
Chew K. W., Wu K., Tassiopoulos K., et al. Liver inflammation is common and linked to metabolic derangements in persons with treated human immunodeficiency virus (HIV). Clin Infect Dis 2023;76(3):e571-79. [PMID: 36049028]
Currier J. S., Taylor A., Boyd F., et al. Coronary heart disease in HIV-infected individuals. J Acquir Immune Defic Syndr 2003;33(4):506-12. [PMID: 12869840]
DHHS. Guidelines for the use of antiretroviral agents in adults and adolescents with HIV: laboratory testing for initial assessment and monitoring of people with HIV receiving antiretroviral therapy. 2022 Sep 21. https://clinicalinfo.hiv.gov/en/guidelines/hiv-clinical-guidelines-adult-and-adolescent-arv/tests-initial-assessment-follow-up [accessed 2024 Aug 5]
DHHS. Guidelines for the use of antiretroviral agents in adults and adolescents with HIV. 2024 Feb 27. https://clinicalinfo.hiv.gov/en/guidelines/adult-and-adolescent-arv/whats-new-guidelines [accessed 2024 Aug 5]
Elion R. A., Althoff K. N., Zhang J., et al. Recent abacavir use increases risk of type 1 and type 2 myocardial infarctions among adults with HIV. J Acquir Immune Defic Syndr 2018;78(1):62-72. [PMID: 29419568]
Erlandson K. M., Carter C. C., Melbourne K., et al. Weight change following antiretroviral therapy switch in people with viral suppression: pooled data from randomized clinical trials. Clin Infect Dis 2021;73(8):1440-51. [PMID: 33987636]
Feinstein M. J., Hsue P. Y., Benjamin L. A., et al. Characteristics, prevention, and management of cardiovascular disease in people living with HIV: a scientific statement from the American Heart Association. Circulation 2019;140(2):e98-124. [PMID: 31154814]
Fichtenbaum C. J., Malvestutto C. D., Watanabe M. G., et al. Abacavir is associated with elevated risk of cardiovascular events in the REPRIEVE trial. Abstract OAB3406LB. 25th International AIDS Conference; 2024 Jul 20-26; Munich, Germany. https://plus.iasociety.org/webcasts/co-morbidities-heart-matter
Freiberg M. S., Chang C. C., Kuller L. H., et al. HIV infection and the risk of acute myocardial infarction. JAMA Intern Med 2013;173(8):614-22. [PMID: 23459863]
Friis-Moller N., Reiss P., Sabin C. A., et al. Class of antiretroviral drugs and the risk of myocardial infarction. N Engl J Med 2007;356(17):1723-35. [PMID: 17460226]
Galizzi N., Galli L., Poli A., et al. Glomerular filtration rate estimated by cystatin C formulas in HIV-1 patients treated with dolutegravir, rilpivirine or cobicistat. New Microbiol 2018;41(4):256-61. [PMID: 30252923]
Gillis J., Bayoumi A. M., Burchell A. N., et al. Factors associated with the frequency of monitoring of liver enzymes, renal function and lipid laboratory markers among individuals initiating combination antiretroviral therapy: a cohort study. BMC Infect Dis 2015;15:453. [PMID: 26496954]
Grinspoon S. K., Fitch K. V., Zanni M. V., et al. Pitavastatin to prevent cardiovascular disease in HIV infection. N Engl J Med 2023;389(8):687-99. [PMID: 37486775]
Gudina E. K., Teklu A. M., Berhan A., et al. Magnitude of antiretroviral drug toxicity in adult HIV patients in Ethiopia: a cohort study at seven teaching hospitals. Ethiop J Health Sci 2017;27(Suppl 1):39-52. [PMID: 28465652]
Hall A. M., Hendry B. M., Nitsch D., et al. Tenofovir-associated kidney toxicity in HIV-infected patients: a review of the evidence. Am J Kidney Dis 2011;57(5):773-80. [PMID: 21435764]
Hirsch K. G., Abella B. S., Amorim E., et al. Critical care management of patients after cardiac arrest: a scientific statement from the American Heart Association and Neurocritical Care Society. Neurocrit Care 2024;40(1):1-37. [PMID: 38040992]
Holt S. G., Gracey D. M., Levy M. T., et al. A consensus statement on the renal monitoring of Australian patients receiving tenofovir based antiviral therapy for HIV/HBV infection. AIDS Res Ther 2014;11:35. [PMID: 25745499]
Jaschinski N., Greenberg L., Neesgaard B., et al. Recent abacavir use and incident cardiovascular disease in contemporary-treated people with HIV. AIDS 2023;37(3):467-75. [PMID: 36001525]
Kalra D. K., Vorla M., Michos E. D., et al. Dyslipidemia in human immunodeficiency virus disease: JACC review topic of the week. J Am Coll Cardiol 2023;82(2):171-81. [PMID: 37407116]
Lake J. E., Wu K., Bares S. H., et al. Risk factors for weight gain following switch to integrase inhibitor-based antiretroviral therapy. Clin Infect Dis 2020;71(9):e471-77. [PMID: 32099991]
Mallon P. W., Brunet L., Hsu R. K., et al. Weight gain before and after switch from TDF to TAF in a U.S. cohort study. J Int AIDS Soc 2021;24(4):e25702. [PMID: 33838004]
Novick T. K., Choi M. J., Rosenberg A. Z., et al. Tenofovir alafenamide nephrotoxicity in an HIV-positive patient: a case report. Medicine (Baltimore) 2017;96(36):e8046. [PMID: 28885375]
O'Halloran J. A., Sahrmann J., Parra-Rodriguez L., et al. Integrase strand transfer inhibitors are associated with incident diabetes mellitus in people with human immunodeficiency virus. Clin Infect Dis 2022;75(12):2060-65. [PMID: 35521785]
Rebeiro P. F., Jenkins C. A., Bian A., et al. Risk of incident diabetes mellitus, weight gain, and their relationships with integrase inhibitor-based initial antiretroviral therapy among persons with human immunodeficiency virus in the United States and Canada. Clin Infect Dis 2021;73(7):e2234-42. [PMID: 32936919]
Ryom L., Lundgren J. D., El-Sadr W., et al. Cardiovascular disease and use of contemporary protease inhibitors: the D:A:D international prospective multicohort study. Lancet HIV 2018;5(6):e291-300. [PMID: 29731407]
Surial B., Mugglin C., Calmy A., et al. Weight and metabolic changes after switching from tenofovir disoproxil fumarate to tenofovir alafenamide in people living with HIV: a cohort study. Ann Intern Med 2021;174(6):758-67. [PMID: 33721521]
Thompson M. A., Horberg M. A., Agwu A. L., et al. Primary care guidance for persons with human immunodeficiency virus: 2020 update by the HIV Medicine Association of the Infectious Diseases Society of America. Clin Infect Dis 2021;73(11):e3572-3605. [PMID: 33225349]
UpToDate. Patient monitoring during HIV antiretroviral therapy. 2023 Mar 31. https://www.uptodate.com/contents/patient-monitoring-during-hiv-antiretroviral-therapy [accessed 2024 Aug 5]
van Wyk J., Ait-Khaled M., Santos J., et al. Brief report: improvement in metabolic health parameters at week 48 after switching from a tenofovir alafenamide-based 3- or 4-drug regimen to the 2-drug regimen of dolutegravir/lamivudine: the TANGO study. J Acquir Immune Defic Syndr 2021;87(2):794-800. [PMID: 33587500]
Venter W. D. F., Sokhela S., Simmons B., et al. Dolutegravir with emtricitabine and tenofovir alafenamide or tenofovir disoproxil fumarate versus efavirenz, emtricitabine, and tenofovir disoproxil fumarate for initial treatment of HIV-1 infection (ADVANCE): week 96 results from a randomised, phase 3, non-inferiority trial. Lancet HIV 2020;7(10):e666-76. [PMID: 33010240]
Yukawa S., Watanabe D., Uehira T., et al. Clinical benefits of using inulin clearance and cystatin C for determining glomerular filtration rate in HIV-1-infected individuals treated with dolutegravir. J Infect Chemother 2018;24(3):199-205. [PMID: 29150412]
Updates, Authorship, and Related Guidelines
| Updates, Authorship, and Related Guidelines | |
| Date of original publication | September 10, 2019 |
| Date of current publication | November 22, 2024 |
| Highlights of changes, additions, and updates in the November 22, 2024 edition |
|
| Intended users | Clinicians providing ambulatory care for patients with HIV |
| Lead author |
Shauna Gunaratne, MD, MPH, DTM&H |
| Writing group |
Rona M. Vail, MD, AAHIVS; Sanjiv S. Shah, MD, MPH, AAHIVS; Steven M. Fine, MD, PhD; Joseph P. McGowan, MD, FACP, FIDSA, AAHIVS; Samuel T. Merrick, MD, FIDSA; Asa E. Radix, MD, MPH, PhD, FACP, AAHIVS; Anne K. Monroe, MD, MSPH; Jessica Rodrigues, MPH, MS; Christopher J. Hoffmann, MD, MPH, MSc, FACP; Brianna L. Norton, DO, MPH; Charles J. Gonzalez, MD |
| Author and writing group conflict of interest disclosures | There are no author or writing group conflict of interest disclosures. |
| Committee | |
| Developer and funder |
New York State Department of Health AIDS Institute (NYSDOH AI) |
| Development process |
See Guideline Development and Recommendation Ratings Scheme, below. |
| Related NYSDOH AI guidelines |
GuidelinePodcast |
Guideline Development and Recommendation Ratings
| Guideline Development: New York State Department of Health AIDS Institute Clinical Guidelines Program | |
| Program manager | Clinical Guidelines Program, Johns Hopkins University School of Medicine, Division of Infectious Diseases. See Program Leadership and Staff. |
| Mission | To produce and disseminate evidence-based, state-of-the-art clinical practice guidelines that establish uniform standards of care for practitioners who provide prevention or treatment of HIV, viral hepatitis, other sexually transmitted infections, and substance use disorders for adults throughout New York State in the wide array of settings in which those services are delivered. |
| Expert committees | The NYSDOH AI Medical Director invites and appoints committees of clinical and public health experts from throughout New York State to ensure that the guidelines are practical, immediately applicable, and meet the needs of care providers and stakeholders in all major regions of New York State, all relevant clinical practice settings, key New York State agencies, and community service organizations. |
| Committee structure |
|
| Disclosure and management of conflicts of interest |
|
| Evidence collection and review |
|
| Recommendation development |
|
| Review and approval process |
|
| External reviews |
|
| Update process |
|
| Recommendation Ratings Scheme | |||
| Strength | Quality of Evidence | ||
| Rating | Definition | Rating | Definition |
| A | Strong | 1 | Based on published results of at least 1 randomized clinical trial with clinical outcomes or validated laboratory endpoints. |
| B | Moderate | * | Based on either a self-evident conclusion; conclusive, published, in vitro data; or well-established practice that cannot be tested because ethics would preclude a clinical trial. |
| C | Optional | 2 | Based on published results of at least 1 well-designed, nonrandomized clinical trial or observational cohort study with long-term clinical outcomes. |
| 2† | Extrapolated from published results of well-designed studies (including nonrandomized clinical trials) conducted in populations other than those specifically addressed by a recommendation. The source(s) of the extrapolated evidence and the rationale for the extrapolation are provided in the guideline text. One example would be results of studies conducted predominantly in a subpopulation (e.g., one gender) that the committee determines to be generalizable to the population under consideration in the guideline. | ||
| 3 | Based on committee expert opinion, with rationale provided in the guideline text. | ||
Last updated on March 24, 2026

