Purpose of This Guideline
Date of current publication: November 4, 2022
Lead author: Meera Shah, MD, MPH, MS, AAHIVS
Contributors: Maria Teresa (Tess) Timoney, MS, RN, CNM, and Jessica M. Atrio, MD, MSc
Writing group: Steven M. Fine, MD, PhD; Rona M. Vail, MD; Joseph P. McGowan, MD, FACP, FIDSA; Samuel T. Merrick, MD; Asa E. Radix, MD, MPH, PhD; Charles J. Gonzalez, MD; Christopher J. Hoffmann, MD, MPH
Committee: Medical Care Criteria Committee
Date of original publication: July 10, 2018
This guideline on human papillomavirus (HPV) in individuals with HIV was developed by the New York State Department of Health AIDS Institute (NYSDOH AI) to inform primary care providers and other practitioners in New York State about HPV prevention, screening methods, diagnosis and presentation, and treatment in adults with HIV. This guideline aims to achieve the following goals:
- Increase the number of New York State residents with HIV who are screened and effectively treated for HPV-related dysplasia.
- Support the NYSDOH Prevention Agenda 2019-2024 by educating care providers on the importance of HPV vaccination and increasing the rate of 3-dose HPV immunization among individuals with HIV.
- Reduce the morbidity and mortality associated with HPV in people with HIV through early identification and treatment of potentially precancerous and cancerous lesions, when treatment is most likely to be effective.
Note on “experienced” HIV care providers: The NYSDOH AI Clinical Guidelines Program defines an “experienced HIV care provider” as a practitioner who has been accorded HIV Specialist status by the American Academy of HIV Medicine. Nurse practitioners (NPs) and licensed midwives who provide clinical care to individuals with HIV in collaboration with a physician may be considered experienced HIV care providers if all other practice agreements are met; NPs with more than 3,600 hours of qualifying experience do not require collaboration with a physician (8 NYCRR 79-5:1; 10 NYCRR 85.36; 8 NYCRR 139-6900). Physician assistants who provide clinical care to individuals with HIV under the supervision of an HIV Specialist physician may also be considered experienced HIV care providers (10 NYCRR 94.2).
HPV-Associated Cancers
HPV-associated cancers: Cervical cancer rates have decreased because of a robust screening system in the United States that has been in place since the 1960s NCI(a) 2022. The incidence of anal cancer persists, particularly among men who have sex with men (MSM) with or without HIV and among women with HIV Islami, et al. 2017; Palefsky 2017; Hessol, et al. 2013, and approximately 91% of anal cancers are thought to be caused by human papillomavirus (HPV) CDC(b) 2022.
This committee has recommended anal screening for specific subpopulations of individuals with HIV since 2007 and recently expanded the recommendation to include anal cytology screening for MSM, cisgender women, transgender women, and transgender men who have HIV and are ≥35 years old. Anal Cancer HSIL Outcomes Research (ANCHOR) study investigators announced by press release in October 2021 that treatment of precancerous lesions reduced anal cancer risk among people with HIV ANCHOR 2021. Although screening tests are available for oropharyngeal cancers, the utility and benefits have not been established; therefore, screening other than visual inspection is not yet recommended (see American Dental Association: Evaluation of Potentially Malignant Disorders in the Oral Cavity Clinical Practice Guideline [2017] for more information). There are no routine screening tests or procedures for vulvar, vaginal, or penile cancers.
HPV types: There are many HPV types, some of which cause cancer (oncogenic) and others of which cause noncancerous disease (nononcogenic verruca vulgaris and condyloma acuminata). Approximately 30 different HPV types infect cells in the anus and genital tract, including the cervix, and may cause asymptomatic infection, condylomata acuminata (genital warts), squamous intraepithelial lesions (SILs), glandular cell abnormalities, and anal and cervical cancer or other genital carcinomas. HPV is also associated with oropharyngeal cancer CDC(a) 2022; CDC(b) 2022. HPV infection is often asymptomatic, and the time course from initial infection to the presence of lesions has not been determined, preventing a reliable method for determining the source and time of acquisition.
In the general U.S. population, HPV types 16 and 18 are responsible for approximately 70% of cases of cervical and anal SILs and cervical and anal cancers Lowy and Schiller 2012; Steinbrook 2006 in addition to most oropharyngeal, vaginal, vulvar, and penile cancers Saraiya, et al. 2015; Forman, et al. 2012; Grulich, et al. 2010; Bouvard, et al. 2009. Nononcogenic HPV types 6 and 11 cause >90% of genital warts CDC(a) 2021; Workowski, et al. 2021. A wider range and higher prevalence of HPV types responsible for oncogenic and nononcogenic disease have been documented in people with HIV Massad, et al. 2016; Kojic, et al. 2011; Clifford, et al. 2006. HPV-associated cancers occur more often among people with HIV than in the general population Liu, et al. 2018; Jemal, et al. 2013, and the distribution of HPV types responsible for SILs and warts also differs between these populations Clifford, et al. 2006.
High-risk HPV types that are related to anogenital cancers include types 16, 18, 26, 31, 33, 35, 39, 45, 51, 52, 53, 56, 58, 59, 66, 67, 68, 69, 70, 73, and 82 Guan, et al. 2012; Hariri, et al. 2012. Although high-risk HPV types are detected in 99% of cervical cancers, types 16 and 18 are the most oncogenic Clifford, et al. 2017; Keller, et al. 2015 and account for nearly 70% of all cervical cancers in the general population CDC(a) 2021. HPV type 16 is the most common high-risk type among individuals with or without HIV Lin, et al. 2018. Among individuals with HIV, cervical cancer is associated with types 16 and 18 and high-risk types 51, 52, 53, 56, 58, and 59 McKenzie, et al. 2010. High-risk HPV types other than type 16 are more common and are more frequently associated with anal cancer among MSM with HIV than MSM without HIV Poynten, et al. 2021. Infection with more than one HPV type occurs more frequently among individuals with HIV, and these individuals can be at risk of cervical and anal SILs and nonmalignant disease simultaneously Castilho, et al. 2015; Clifford, et al. 2006.
Tobacco use: Tobacco use is an established contributor to the oncogenic potential of HPV and is an independent risk factor for acquisition and progression of cervical SILs Collins, et al. 2010, anal neoplasia Daling, et al. 2004, oropharyngeal cancer NCI(b) 2022, and vulvar cancer in individuals with HIV ACS 2018; Kutlubay, et al. 2013. Some data suggest that HIV-related immune suppression can contribute to relapse and progression of HPV disease, and antiretroviral therapy-mediated immune reconstitution can lead to regression of SILs associated with HPV infection Blitz, et al. 2013. Other studies do not support this finding Piketty, et al. 2013; Adler 2010.
HPV Prevention
| RECOMMENDATION |
HPV Prevention
|
HPV Vaccine
In 2006, the U.S. Food and Drug Administration (FDA) approved a 9-valent vaccine that protects against nononcogenic HPV types 16, 18, 31, 33, 45, 52, and 58 (Gardasil 9). Because it offers broader coverage of HPV types, the 9-valent vaccine is the only HPV vaccine available in the United States (see CDC supplemental information and guidance for vaccination providers regarding use of 9-valent HPV for more information). The HPV vaccine is approved by the FDA for preventive but not therapeutic use.
Extrapolating data from the demonstrated effectiveness of the quadrivalent HPV vaccine in older individuals Wilkin, et al. 2018, the FDA expanded the age range for recommended HPV vaccination in the United States from ages 9 to 26 years to ages 27 to 45 years FDA 2020. There is no specific mention of HIV infection in the updated FDA recommendation. Although 1 study demonstrated lower efficacy of the quadrivalent vaccine in individuals with HIV Wilkin, et al. 2018, other research linked HIV viral suppression to vaccine efficacy Money, et al. 2016. Given the increased lifetime burden of persistent HPV infection, disease, and morbidity, proactive vaccination among individuals with HIV is a strategic means of primary prevention and potential disease mitigation that should be strongly considered and encouraged Di Donato, et al. 2021; Karimi-Zarchi, et al. 2020; Lichter, et al. 2020.
When to Vaccinate
HPV vaccination may be scheduled at the same time as standard adolescent vaccines offered at ages 9 to 12 years. If possible, the vaccine series should begin at age 9 years Glidden, et al. 2016. The 3-dose vaccine regimen is recommended for all patients with HIV who are 9 to 45 years old. The 9-valent HPV vaccine should be administered according to the CDC standard schedule for immunocompromised adults, children, and adolescents (a 3-dose regimen over a 6-month period at 0, 2, and 6 months) and should be offered regardless of CD4 cell count.
HPV vaccination provides high levels of neutralizing antibody for at least 5 years and is protective in individuals ≤26 years old who do not have HIV, regardless of history of sexual activity; however, the full length of its protection has not been established. In an observational study conducted in England that examined the effectiveness of a national HPV immunization program, the reduction in cervical cancer was greatest in individuals who received the vaccine at ages 12 to 13 years Falcaro, et al. 2021. Although data are limited, the immunogenicity of the quadrivalent HPV vaccine has been demonstrated in individuals with HIV Wilkin, et al. 2018; Kojic, et al. 2014.
HPV testing and vaccination: HPV testing is not recommended before vaccine administration. It is unlikely that an individual will have been infected with all the HPV types covered by the 9-valent vaccine; therefore, it is expected that the 9-valent HPV vaccine will be effective against any of the 9 HPV types or any HPV types to which the individual has not been exposed. There also may be beneficial prevention due to cross-reactivity with other HPV types not included in the 9-valent vaccine Wheeler, et al. 2012.
Revaccination with the 9-valent HPV vaccine is not currently recommended for individuals previously immunized with the bivalent or quadrivalent HPV vaccine ACOG 2020; Petrosky, et al. 2015. Vaccination with the quadrivalent HPV vaccine has demonstrated cross-protection against other oncogenic HPV types Kemp, et al. 2011. There is no maximum interval between vaccine doses; as long as all 3 doses are given, there is no need to repeat doses if a scheduled vaccination is not given on schedule CDC(b) 2021.
| KEY POINT |
|
Other Forms of HPV Prevention
HPV infection is the most common sexually transmitted infection (STI) in the United States, and many individuals become infected with multiple types of HPV during their lives CDC(c) 2021. Most HPV infections resolve, become latent, or are not detectable on clinical assays within a few years of exposure and infection Ho, et al. 1998; Moscicki, et al. 1998; Evander, et al. 1995. HPV is transmitted via skin-to-skin contact, so barrier methods such as condoms offer some but not full protection. Because prior identification of HPV infection in a sexual partner is unlikely, limiting the number of sexual partners may reduce but not eliminate an individual’s exposure to HPV Workowski, et al. 2021.
| KEY POINTS |
|
Cervical and Anal Cancer Screening
| RECOMMENDATIONS |
Cervical and Anal Cancer Screening
|
Cervical cancer screening: Clinicians should perform cervical and anal cytologic screening for people with HIV according to the recommendations in the NYSDOH AI guidelines Screening for Cervical Dysplasia and Cancer in Adults With HIV and Screening for Anal Dysplasia and Cancer in Adults With HIV. HPV testing with cytologic screening enhances the identification of HPV-related cervical disease in individuals with HIV. Examination of the anogenital area of patients with HIV to assess for visible HPV lesions is necessary because HPV can also infect the urethra and the external genitalia Ehrenpreis and Smith 2018; Leeds and Fang 2016; Tyerman and Aboulafia 2012; Weyers, et al. 2010. Speculum examination of the vagina, neovagina, and cervix and anoscopic examination of the anus and lower rectum may also reveal lesions. There are currently no data on urethral screening and treatment, but referral to a urologist will facilitate appropriate assessment and management when this is a concern.
Anal cancer screening: Anal squamous intraepithelial lesions (SILs) have been associated with concurrent cervical SILs; however, they also occur independently. Anal cytology should be performed for all cisgender women with HIV Gaisa, et al. 2017; Stier, et al. 2015; Hessol, et al. 2013; Kojic, et al. 2011, with or without cervical abnormalities, according to guidelines for adults with HIV. Although there are no specific data on transgender men or transgender women, anal screening is also recommended for these populations.
Transgender individuals: It is important that care providers and facilities establish a safe and welcoming environment for transgender patients UCSF 2016. Approximately one-third of transgender or gender-diverse individuals assigned female sex at birth identify as nonbinary National Center for Transgender Equality 2016. Asking patients to provide details about all gender-affirming and gynecologic surgical procedures will help establish the need for screening for HPV-related cancers. For terminology and definitions related to transgender care, see University of California San Francisco Gender-Affirming Health Program.
Sexual history: Discussion of sexual health, including a patient’s history of sexually transmitted infections (STIs), is an important component of the baseline and annual assessments and is an opportunity to discuss a patient’s concerns and questions. The frequency of the sexual health assessment is based on risk factors. It is particularly important to use nonjudgmental, sex-positive language in this discussion to establish a strong connection and facilitate open discussion.
| KEY POINTS |
|
Presentation and Diagnosis of HPV Infection
| RECOMMENDATIONS |
Presentation and Diagnosis of HPV Infection
|
Abbreviations: HPV, human papillomavirus; HRA, high-resolution anoscopy. |
Diagnosis of external condylomata acuminata is often made based on clinical appearance. The appearance of warts varies. Condylomata acuminata (genital warts) can be smooth and skin-colored or hyperpigmented papules or plaques that may be flat, hyperkeratotic, nodular, or exophytic. Symptoms may be absent or may include itching, bleeding, burning, and discomfort. Warts on the external genitalia and the cervix are commonly flat, plaque-like lesions but may also be exophytic and visible to the naked eye. Cervical lesions are best visualized by colposcopy. Penile lesions can occur along the shaft but may also occur along the penile urethra and be hidden from view.
Small external lesions are often treated without biopsy. Lesions that are atypical or variegated in color or shape require biopsy to exclude squamous intraepithelial lesions (SILs) or cancer. Clinicians should maintain a low threshold for obtaining biopsies of the following, which may indicate precancerous or cancerous lesions: atypical-appearing lesions; pigmented, internal, or condylomatous lesions; rapidly growing lesions; or lesions that fail to respond to standard treatment.
Manifestations of HPV infection in individuals with HIV infection may include the following Wang and Palefsky 2019; Liu, et al. 2018; Clifford, et al. 2017; Palefsky 2017; Lillo, et al. 2001; Minkoff, et al. 2001; Palefsky(a), et al. 2001; Palefsky(b), et al. 2001; Frisch, et al. 2000; Palefsky, et al. 1998:
- Condylomata acuminata, anal SILs, anal intraepithelial neoplasia, cervical SILs, and cervical intraepithelial neoplasia have all been reported to occur more frequently in people with HIV.
- With increased immunosuppression, there is evidence for increased risk of persistent and recurrent HPV infection and disease of the anal and genital tracts; decreased rates of spontaneous disease regression; increased severity of HPV disease; anal SILs and cervical SILs; and development of condylomata acuminata.
- HPV infection may be more difficult to treat and more likely to recur with advanced immunosuppression.
- Patients with more advanced immunosuppression have an increased relative risk of developing HPV-related invasive anogenital cancers.
| Resources |
|
For images of the clinical manifestations of HPV, see the following: |
Data are mixed regarding the contribution of HIV-related immune suppression to the relapse and progression of HPV disease and whether antiretroviral therapy (ART)-mediated immune reconstitution can lead to regression of SIL associated with HPV infection Blitz, et al. 2013; Piketty, et al. 2013; Adler 2010. Although there are cases of involution of mucocutaneous warts after initiation of ART, the prevalence or course of anogenital HPV disease is not altered significantly by ART Lofgren, et al. 2015; Adler 2010.
| KEY POINTS |
|
HPV Treatment
| RECOMMENDATIONS |
HPV Treatment
|
The standard therapeutic approach to treating HPV-related nonmalignant lesions (condyloma/warts) and dysplasia (squamous intraepithelial lesions or above) in individuals with HIV is the same as that for individuals without HIV. Treatment of condyloma is aimed at removing symptomatic visible warts. However, some untreated warts may resolve spontaneously. There has been no evidence that any available treatment regimen eradicates HPV infection. Comparative efficacy trials of the different treatment options for patients with HIV have not been conducted. Treatment of precancerous lesions includes ablation, using cryotherapy or laser, and surgical or laser excision. These procedures should be performed only by experienced clinicians (for more information, see NYSDOH AI guideline Screening for Cervical Dysplasia and Cancer in Adults With HIV).
Cryotherapy, electrocautery, podophyllotoxin, interferon, imiquimod, cidofovir gel, trichloroacetic acid, and bichloroacetic acid have all demonstrated efficacy treating anogenital warts in patients without HIV. In a systematic review and meta-analysis, electrocautery and imiquimod were shown to be efficacious in treating anogenital warts in people with HIV Werner, et al. 2017. Controlled studies of other HPV interventions in people with HIV have not been done. Interferon, 5-fluorouracil, and podophyllotoxin are no longer preferred HPV treatments in the primary care setting because of low efficacy and toxicity that may limit their routine use Lacey, et al. 2013. The safety and efficacy of sinecatechins have not been evaluated in individuals with HIV and therefore should not be used FDA 2007.
There are limited data on imiquimod use in pregnancy, but animal data suggest low risk of harm Workowski, et al. 2021. This drug can be used during pregnancy if no other options, including waiting until after delivery, are available. Because of a lack of safety data, podophyllin should not be used during pregnancy. Podofilox (podophyllotoxin) is contraindicated in pregnancy Briggs, et al. 2017.
Data on treating HPV lesions of the neovagina, whether penile or colonic in origin, are limited to case reports and small case series. Standard, care provider-applied approaches to treatment should be used Labanca and Mañero 2017; van der Sluis, et al. 2016; Matsuki, et al. 2015; Wasef, et al. 2005; Liguori, et al. 2004; Fiumara and Di Mattia 1973.
Clinicians often report poor clearance rates after therapy in patients with HIV Richel, et al. 2013. More than one application of therapy, more than one method of treatment (e.g., topical imiquimod followed by cryotherapy), or longer duration of treatment is often needed. Treatment length may vary, and frequent visits (as often as biweekly) are necessary to assess lesion regression and adverse effects. Topical treatments may cause adverse effects such as irritation and a burning sensation, which may affect treatment adherence. The response to treatment and its adverse effects should be evaluated throughout the course of therapy. The treatment approach may need to be changed if a patient has not improved substantially after standard therapy. There are no data available regarding effects of HPV treatment on HPV transmissibility.
When deciding whether to treat a patient with HIV for anogenital warts or refer the patient to a specialist, clinicians should consider their own experience and available resources, diagnostic certainty, anatomic site of lesions, potential adverse effects of treatment, and the patient’s ability to adhere to treatment.
Table 1, below, lists available treatment options for condyloma for patients with HIV.
| Table 1: Available Treatment Options for Anogenital Condyloma for Patients With HIV [a] | ||
| Abbreviations: BCA, bichloroacetic acid; TCA, trichloroacetic acid.
Notes:
|
||
| Condyloma Type | Treatment [b,c] | Comments |
| Anogenital condyloma |
Patient self-administered treatments:
|
|
| Urethral meatus condyloma |
|
— |
| Vaginal condyloma |
|
Cryoprobe use in the vagina is not recommended because of the risk of vaginal perforation and fistula formation. |
| Cervical condyloma |
|
|
| Intra-anal condyloma |
|
Management of intra-anal warts should include consultation with a colorectal specialist. |
| Neovaginal condyloma [f,g] |
Patient self-administered treatments:
|
Imiquimod may weaken condoms and vaginal diaphragms. |
Partner Exposure to HIV and HPV
| RECOMMENDATION |
Partner Exposure to HIV and HPV
|
Treatment of lesions solely for the prevention of future transmission cannot be recommended because the value of treatment in reducing infectivity is not known. However, sex partners of patients who have genital lesions might benefit from counseling and examination to assess the presence of genital warts and HPV-related dysplasia. Sex partners should also be evaluated for other sexually transmitted infections (STIs), including HIV, because HPV disease is transmitted sexually Workowski, et al. 2021.
Clinicians should inform patients that any sex partner who does not have confirmed HIV infection should have routine HIV testing for early identification of HIV acquisition. If a patient with an HIV exposure presents within 36 hours, evaluation for non-occupational post-exposure prophylaxis (PEP) should occur. When possible, onsite availability of HIV testing and STI treatment for partners is ideal because it may increase the likelihood that partners will receive timely access to HIV testing and appropriate treatment, including HIV PEP and treatment for the STI as needed. Such strategies may also increase identification of individuals who require ongoing medical care. Partner education about reducing high-risk sexual behaviors, including counseling about the use of male/insertive and female/receptive condoms and making condoms visibly available in the clinic, may help further decrease the risk of transmission of both HIV and other STIs. Patients who remain at high risk of exposure after completing a course of non-occupational PEP and who are negative for HIV at the time of the 4-week test should be offered pre-exposure prophylaxis (PrEP), to begin immediately after the last dose of non-occupational PEP. Patient education about undetectable=untransmittable (U=U) as an HIV prevention strategy should stress that an undetectable HIV viral load prevents only the sexual transmission of HIV.
| New York State Law |
|
The NYSDOH Partner Services program provides assistance to individuals with HIV and care providers who would like help notifying a patient’s sex partner(s) of possible exposure to HIV, chlamydia, gonorrhea, or syphilis. Available options for partner notification include anonymous notification from the local health department, dual disclosure (patient disclosure with the help of Partner Services staff), and self-disclosure. Partner Services staff within local health departments work with patients to develop a plan to notify their partners, whether that plan includes staff notifying potentially exposed partners anonymously or helping patients who choose to tell their partners on their own develop a notification plan and strategy.
| KEY POINTS |
|
All Recommendations
| ALL RECOMMENDATIONS: PREVENTION AND MANAGEMENT OF HUMAN PAPILLOMAVIRUS INFECTION IN ADULTS WITH HIV |
HPV Prevention
Cervical and Anal Cancer Screening
Presentation and Diagnosis of HPV Infection
HPV Treatment
Partner Exposure to HIV and HPV
|
Abbreviations: HPV, human papillomavirus; HRA, high-resolution anoscopy. |
Shared Decision-Making
Download Printable PDF of Shared Decision-Making Statement
Date of current publication: August 8, 2023
Lead authors: Jessica Rodrigues, MS; Jessica M. Atrio, MD, MSc; and Johanna L. Gribble, MA
Writing group: Steven M. Fine, MD, PhD; Rona M. Vail, MD; Samuel T. Merrick, MD; Asa E. Radix, MD, MPH, PhD; Christopher J. Hoffmann, MD, MPH; Charles J. Gonzalez, MD
Committee: Medical Care Criteria Committee
Date of original publication: August 8, 2023
Rationale
Throughout its guidelines, the New York State Department of Health (NYSDOH) AIDS Institute (AI) Clinical Guidelines Program recommends “shared decision-making,” an individualized process central to patient-centered care. With shared decision-making, clinicians and patients engage in meaningful dialogue to arrive at an informed, collaborative decision about a patient’s health, care, and treatment planning. The approach to shared decision-making described here applies to recommendations included in all program guidelines. The included elements are drawn from a comprehensive review of multiple sources and similar attempts to define shared decision-making, including the Institute of Medicine’s original description [Institute of Medicine 2001]. For more information, a variety of informative resources and suggested readings are included at the end of the discussion.
Benefits
The benefits to patients that have been associated with a shared decision-making approach include:
- Decreased anxiety [Niburski, et al. 2020; Stalnikowicz and Brezis 2020]
- Increased trust in clinicians [Acree, et al. 2020; Groot, et al. 2020; Stalnikowicz and Brezis 2020]
- Improved engagement in preventive care [McNulty, et al. 2022; Scalia, et al. 2022; Bertakis and Azari 2011]
- Improved treatment adherence, clinical outcomes, and satisfaction with care [Crawford, et al. 2021; Bertakis and Azari 2011; Robinson, et al. 2008]
- Increased knowledge, confidence, empowerment, and self-efficacy [Chen, et al. 2021; Coronado-Vázquez, et al. 2020; Niburski, et al. 2020]
Approach
Collaborative care: Shared decision-making is an approach to healthcare delivery that respects a patient’s autonomy in responding to a clinician’s recommendations and facilitates dynamic, personalized, and collaborative care. Through this process, a clinician engages a patient in an open and respectful dialogue to elicit the patient’s knowledge, experience, healthcare goals, daily routine, lifestyle, support system, cultural and personal identity, and attitudes toward behavior, treatment, and risk. With this information and the clinician’s clinical expertise, the patient and clinician can collaborate to identify, evaluate, and choose from among available healthcare options [Coulter and Collins 2011]. This process emphasizes the importance of a patient’s values, preferences, needs, social context, and lived experience in evaluating the known benefits, risks, and limitations of a clinician’s recommendations for screening, prevention, treatment, and follow-up. As a result, shared decision-making also respects a patient’s autonomy, agency, and capacity in defining and managing their healthcare goals. Building a clinician-patient relationship rooted in shared decision-making can help clinicians engage in productive discussions with patients whose decisions may not align with optimal health outcomes. Fostering open and honest dialogue to understand a patient’s motivations while suspending judgment to reduce harm and explore alternatives is particularly vital when a patient chooses to engage in practices that may exacerbate or complicate health conditions [Halperin, et al. 2007].
Options: Implicit in the shared decision-making process is the recognition that the “right” healthcare decisions are those made by informed patients and clinicians working toward patient-centered and defined healthcare goals. When multiple options are available, shared decision-making encourages thoughtful discussion of the potential benefits and potential harms of all options, which may include doing nothing or waiting. This approach also acknowledges that efficacy may not be the most important factor in a patient’s preferences and choices [Sewell, et al. 2021].
Clinician awareness: The collaborative process of shared decision-making is enhanced by a clinician’s ability to demonstrate empathic interest in the patient, avoid stigmatizing language, employ cultural humility, recognize systemic barriers to equitable outcomes, and practice strategies of self-awareness and mitigation against implicit personal biases [Parish, et al. 2019].
Caveats: It is important for clinicians to recognize and be sensitive to the inherent power and influence they maintain throughout their interactions with patients. A clinician’s identity and community affiliations may influence their ability to navigate the shared decision-making process and develop a therapeutic alliance with the patient and may affect the treatment plan [KFF 2023; Greenwood, et al. 2020]. Furthermore, institutional policy and regional legislation, such as requirements for parental consent for gender-affirming care for transgender people or insurance coverage for sexual health care, may infringe upon a patient’s ability to access preventive- or treatment-related care [Sewell, et al. 2021].
Figure 1: Elements of Shared Decision-Making
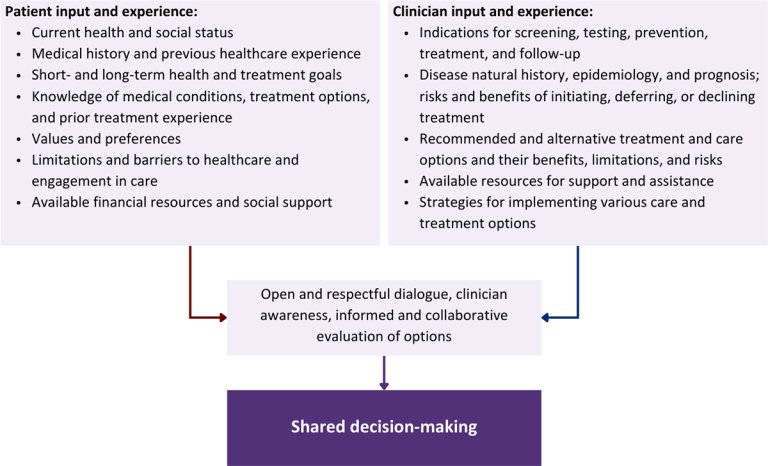
Health equity: Adapting a shared decision-making approach that supports diverse populations is necessary to achieve more equitable and inclusive health outcomes [Castaneda-Guarderas, et al. 2016]. For instance, clinicians may need to incorporate cultural- and community-specific considerations into discussions with women, gender-diverse individuals, and young people concerning their sexual behaviors, fertility intentions, and pregnancy or lactation status. Shared decision-making offers an opportunity to build trust among marginalized and disenfranchised communities by validating their symptoms, values, and lived experience. Furthermore, it can allow for improved consistency in patient screening and assessment of prevention options and treatment plans, which can reduce the influence of social constructs and implicit bias [Castaneda-Guarderas, et al. 2016].
Clinician bias has been associated with health disparities and can have profoundly negative effects [FitzGerald and Hurst 2017; Hall, et al. 2015]. It is often challenging for clinicians to recognize and set aside personal biases and to address biases with peers and colleagues. Consciously or unconsciously, negative or stigmatizing assumptions are often made about patient characteristics, such as race, ethnicity, gender, sexual orientation, mental health, and substance use [Avery, et al. 2019; van Boekel, et al. 2013; Livingston, et al. 2012]. With its emphasis on eliciting patient information, a shared decision-making approach encourages clinicians to inquire about patients’ lived experiences rather than making assumptions and to recognize the influence of that experience in healthcare decision-making.
Stigma: Stigma may prevent individuals from seeking or receiving treatment and harm reduction services [Tsai, et al. 2019]. Among people with HIV, stigma and medical mistrust remain significant barriers to healthcare utilization, HIV diagnosis, and medication adherence and can affect disease outcomes [Turan, et al. 2017; Chambers, et al. 2015], and stigma among clinicians against people who use substances has been well-documented [Stone, et al. 2021; Tsai, et al. 2019; van Boekel, et al. 2013]. Sexual and reproductive health, including strategies to prevent HIV transmission, acquisition, and progression, may be subject to stigma, bias, social influence, and violence.
| SHARED DECISION-MAKING IN HIV CARE |
|
Resources and Suggested Reading
In addition to the references cited below, the following resources and suggested reading may be useful to clinicians.
| RESOURCES |
References
Acree ME, McNulty M, Blocker O, et al. Shared decision-making around anal cancer screening among black bisexual and gay men in the USA. Cult Health Sex 2020;22(2):201-16. [PMID: 30931831]
Avery JD, Taylor KE, Kast KA, et al. Attitudes toward individuals with mental illness and substance use disorders among resident physicians. Prim Care Companion CNS Disord 2019;21(1):18m02382. [PMID: 30620451]
Bertakis KD, Azari R. Patient-centered care is associated with decreased health care utilization. J Am Board Fam Med 2011;24(3):229-39. [PMID: 21551394]
Castaneda-Guarderas A, Glassberg J, Grudzen CR, et al. Shared decision making with vulnerable populations in the emergency department. Acad Emerg Med 2016;23(12):1410-16. [PMID: 27860022]
Chambers LA, Rueda S, Baker DN, et al. Stigma, HIV and health: a qualitative synthesis. BMC Public Health 2015;15:848. [PMID: 26334626]
Chen CH, Kang YN, Chiu PY, et al. Effectiveness of shared decision-making intervention in patients with lumbar degenerative diseases: a randomized controlled trial. Patient Educ Couns 2021;104(10):2498-2504. [PMID: 33741234]
Coronado-Vázquez V, Canet-Fajas C, Delgado-Marroquín MT, et al. Interventions to facilitate shared decision-making using decision aids with patients in primary health care: a systematic review. Medicine (Baltimore) 2020;99(32):e21389. [PMID: 32769870]
Coulter A, Collins A. Making shared decision-making a reality: no decision about me, without me. 2011. https://www.kingsfund.org.uk/sites/default/files/Making-shared-decision-making-a-reality-paper-Angela-Coulter-Alf-Collins-July-2011_0.pdf
Crawford J, Petrie K, Harvey SB. Shared decision-making and the implementation of treatment recommendations for depression. Patient Educ Couns 2021;104(8):2119-21. [PMID: 33563500]
FitzGerald C, Hurst S. Implicit bias in healthcare professionals: a systematic review. BMC Med Ethics 2017;18(1):19. [PMID: 28249596]
Greenwood BN, Hardeman RR, Huang L, et al. Physician-patient racial concordance and disparities in birthing mortality for newborns. Proc Natl Acad Sci U S A 2020;117(35):21194-21200. [PMID: 32817561]
Groot G, Waldron T, Barreno L, et al. Trust and world view in shared decision making with indigenous patients: a realist synthesis. J Eval Clin Pract 2020;26(2):503-14. [PMID: 31750600]
Hall WJ, Chapman MV, Lee KM, et al. Implicit racial/ethnic bias among health care professionals and its influence on health care outcomes: a systematic review. Am J Public Health 2015;105(12):e60-76. [PMID: 26469668]
Halperin B, Melnychuk R, Downie J, et al. When is it permissible to dismiss a family who refuses vaccines? Legal, ethical and public health perspectives. Paediatr Child Health 2007;12(10):843-45. [PMID: 19043497]
Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. 2001. https://www.ncbi.nlm.nih.gov/books/NBK222274/
KFF. Key data on health and health care by race and ethnicity. 2023 Mar 15. https://www.kff.org/racial-equity-and-health-policy/report/key-data-on-health-and-health-care-by-race-and-ethnicity/ [accessed 2023 May 19]
Livingston JD, Milne T, Fang ML, et al. The effectiveness of interventions for reducing stigma related to substance use disorders: a systematic review. Addiction 2012;107(1):39-50. [PMID: 21815959]
McNulty MC, Acree ME, Kerman J, et al. Shared decision making for HIV pre-exposure prophylaxis (PrEP) with black transgender women. Cult Health Sex 2022;24(8):1033-46. [PMID: 33983866]
Niburski K, Guadagno E, Abbasgholizadeh-Rahimi S, et al. Shared decision making in surgery: a meta-analysis of existing literature. Patient 2020;13(6):667-81. [PMID: 32880820]
Parish SJ, Hahn SR, Goldstein SW, et al. The International Society for the Study of Women’s Sexual Health process of care for the identification of sexual concerns and problems in women. Mayo Clin Proc 2019;94(5):842-56. [PMID: 30954288]
Robinson JH, Callister LC, Berry JA, et al. Patient-centered care and adherence: definitions and applications to improve outcomes. J Am Acad Nurse Pract 2008;20(12):600-607. [PMID: 19120591]
Scalia P, Durand MA, Elwyn G. Shared decision-making interventions: an overview and a meta-analysis of their impact on vaccine uptake. J Intern Med 2022;291(4):408-25. [PMID: 34700363]
Sewell WC, Solleveld P, Seidman D, et al. Patient-led decision-making for HIV preexposure prophylaxis. Curr HIV/AIDS Rep 2021;18(1):48-56. [PMID: 33417201]
Stalnikowicz R, Brezis M. Meaningful shared decision-making: complex process demanding cognitive and emotional skills. J Eval Clin Pract 2020;26(2):431-38. [PMID: 31989727]
Stone EM, Kennedy-Hendricks A, Barry CL, et al. The role of stigma in U.S. primary care physicians’ treatment of opioid use disorder. Drug Alcohol Depend 2021;221:108627. [PMID: 33621805]
Tsai AC, Kiang MV, Barnett ML, et al. Stigma as a fundamental hindrance to the United States opioid overdose crisis response. PLoS Med 2019;16(11):e1002969. [PMID: 31770387]
Turan B, Budhwani H, Fazeli PL, et al. How does stigma affect people living with HIV? The mediating roles of internalized and anticipated HIV stigma in the effects of perceived community stigma on health and psychosocial outcomes. AIDS Behav 2017;21(1):283-91. [PMID: 27272742]
van Boekel LC, Brouwers EP, van Weeghel J, et al. Stigma among health professionals towards patients with substance use disorders and its consequences for healthcare delivery: systematic review. Drug Alcohol Depend 2013;131(1-2):23-35. [PMID: 23490450]
References
ACOG. Human papillomavirus vaccination: ACOG committee opinion, number 809. Obstet Gynecol 2020;136(2):e15-e21. [PMID: 32732766]
ACS. Risk factors for vulvar cancer. 2018 Jan 16. https://www.cancer.org/cancer/vulvar-cancer/causes-risks-prevention/risk-factors.html [accessed 2022 Oct 17]
Adler D. H. The impact of HAART on HPV-related cervical disease. Curr HIV Res 2010;8(7):493-97. [PMID: 20946095]
ANCHOR. Press release: treating anal cancer precursor lesions reduces cancer risk for people with HIV. 2021 Oct 7. https://iansoc.org/resources/ANCHOR%20press%20release_07OCT2021.pdf [accessed 2022 Oct 17]
Blitz S., Baxter J., Raboud J., et al. Evaluation of HIV and highly active antiretroviral therapy on the natural history of human papillomavirus infection and cervical cytopathologic findings in HIV-positive and high-risk HIV-negative women. J Infect Dis 2013;208(3):454-62. [PMID: 23624362]
Bouvard V., Baan R., Straif K., et al. A review of human carcinogens--part B: biological agents. Lancet Oncol 2009;10(4):321-22. [PMID: 19350698]
Briggs G. G., Freeman R. K., Yaffe S. J. Drugs in pregnancy and lactation: a reference guide to fetal and neonatal risk. Williams & Wilkins; 2017. https://books.google.com/books?id=o3ymMgEACAAJ
Castilho J. L., Levi J. E., Luz P. M., et al. A cross-sectional study of high-risk human papillomavirus clustering and cervical outcomes in HIV-infected women in Rio de Janeiro, Brazil. BMC Cancer 2015;15:478. [PMID: 26100400]
CDC(a). Epidemiology and prevention of vaccine-preventable diseases: human papillomavirus. 2021 Aug 18. https://www.cdc.gov/vaccines/pubs/pinkbook/hpv.html [accessed 2022 Oct 17]
CDC(a). How many cancers are linked with HPV each year?. 2022 Oct 3. https://www.cdc.gov/cancer/hpv/statistics/cases.htm [accessed 2022 Oct 17]
CDC(b). HPV vaccine schedule and dosing. 2021 Nov 1. https://www.cdc.gov/hpv/hcp/schedules-recommendations.html [accessed 2022 Oct 17]
CDC(b). HPV-associated cancer diagnosis by age. 2022 Oct 3. https://www.cdc.gov/cancer/hpv/statistics/age.htm [accessed 2022 Oct 17]
CDC(c). Sexually transmitted infections prevalence, incidence, and cost estimates in the United States. 2021 Jan 25. https://www.cdc.gov/std/statistics/prevalence-2020-at-a-glance.htm [accessed 2022 Oct 17]
Clifford G. M., Goncalves M. A., Franceschi S. Human papillomavirus types among women infected with HIV: a meta-analysis. AIDS 2006;20(18):2337-44. [PMID: 17117020]
Clifford G. M., Tully S., Franceschi S. Carcinogenicity of human papillomavirus (HPV) types in HIV-positive women: a meta-analysis from HPV infection to cervical cancer. Clin Infect Dis 2017;64(9):1228-35. [PMID: 28199532]
Collins S., Rollason T. P., Young L. S., et al. Cigarette smoking is an independent risk factor for cervical intraepithelial neoplasia in young women: a longitudinal study. Eur J Cancer 2010;46(2):405-11. [PMID: 19819687]
Daling J. R., Madeleine M. M., Johnson L. G., et al. Human papillomavirus, smoking, and sexual practices in the etiology of anal cancer. Cancer 2004;101(2):270-80. [PMID: 15241823]
Di Donato V., Caruso G., Petrillo M., et al. Adjuvant HPV vaccination to prevent recurrent cervical dysplasia after surgical treatment: a meta-analysis. Vaccines (Basel) 2021;9(5). [PMID: 33919003]
Ehrenpreis E. D., Smith D. G. Patients with newly diagnosed cervical cancer should be screened for anal human papilloma virus and anal dysplasia: results of a pilot study using a STELLA computer simulation and economic model. Papillomavirus Res 2018;5:38-45. [PMID: 29272853]
Evander M., Edlund K., Gustafsson A., et al. Human papillomavirus infection is transient in young women: a population-based cohort study. J Infect Dis 1995;171(4):1026-30. [PMID: 7706782]
Falcaro M., Castanon A., Ndlela B., et al. The effects of the national HPV vaccination programme in England, UK, on cervical cancer and grade 3 cervical intraepithelial neoplasia incidence: a register-based observational study. Lancet 2021;398(10316):2084-92. [PMID: 34741816]
FDA. Veregen (sinecatechins) ointment, 15%. 2007 Dec. https://www.accessdata.fda.gov/drugsatfda_docs/label/2007/021902s002lbl.pdf [accessed 2022 Oct 17]
FDA. Gardasil 9. 2020 Aug 21. https://www.fda.gov/vaccines-blood-biologics/vaccines/gardasil-9 [accessed 2022 Oct 17]
Fiumara N. J., Di Mattia A. Gonorrhoea and condyloma acuminata in a male transsexual. Br J Vener Dis 1973;49(5):478-79. [PMID: 4270635]
Forman D., de Martel C., Lacey C. J., et al. Global burden of human papillomavirus and related diseases. Vaccine 2012;30 Suppl 5:F12-23. [PMID: 23199955]
Frisch M., Biggar R. J., Goedert J. J. Human papillomavirus-associated cancers in patients with human immunodeficiency virus infection and acquired immunodeficiency syndrome. J Natl Cancer Inst 2000;92(18):1500-1510. [PMID: 10995805]
Gaisa M., Ita-Nagy F., Sigel K., et al. High rates of anal high-grade squamous intraepithelial lesions in HIV-infected women who do not meet screening guidelines. Clin Infect Dis 2017;64(3):289-294. [PMID: 27965301]
Glidden D. V., Amico K. R., Liu A. Y., et al. Symptoms, side effects and adherence in the iPrEx open-label extension. Clin Infect Dis 2016;62(9):1172-77. [PMID: 26797207]
Grulich A. E., Jin F., Conway E. L., et al. Cancers attributable to human papillomavirus infection. Sex Health 2010;7(3):244-52. [PMID: 20719211]
Guan P., Howell-Jones R., Li N., et al. Human papillomavirus types in 115,789 HPV-positive women: a meta-analysis from cervical infection to cancer. Int J Cancer 2012;131(10):2349-59. [PMID: 22323075]
Hariri S., Unger E. R., Powell S. E., et al. Human papillomavirus genotypes in high-grade cervical lesions in the United States. J Infect Dis 2012;206(12):1878-86. [PMID: 23045628]
Hessol N. A., Holly E. A., Efird J. T., et al. Concomitant anal and cervical human papillomavirusV infections and intraepithelial neoplasia in HIV-infected and uninfected women. AIDS 2013;27(11):1743-51. [PMID: 23803793]
Ho G. Y., Bierman R., Beardsley L., et al. Natural history of cervicovaginal papillomavirus infection in young women. N Engl J Med 1998;338(7):423-28. [PMID: 9459645]
Islami F., Ferlay J., Lortet-Tieulent J., et al. International trends in anal cancer incidence rates. Int J Epidemiol 2017;46(3):924-38. [PMID: 27789668]
Jemal A., Simard E. P., Dorell C., et al. Annual report to the nation on the status of cancer, 1975-2009, featuring the burden and trends in human papillomavirus(HPV)-associated cancers and HPV vaccination coverage levels. J Natl Cancer Inst 2013;105(3):175-201. [PMID: 23297039]
Karimi-Zarchi M., Allahqoli L., Nehmati A., et al. Can the prophylactic quadrivalent HPV vaccine be used as a therapeutic agent in women with CIN? A randomized trial. BMC Public Health 2020;20(1):274. [PMID: 32106837]
Keller M. J., Burk R. D., Massad L. S., et al. Cervical precancer risk in HIV-infected women who test positive for oncogenic human papillomavirus despite a normal pap test. Clin Infect Dis 2015;61(10):1573-81. [PMID: 26187020]
Kemp T. J., Hildesheim A., Safaeian M., et al. HPV16/18 L1 VLP vaccine induces cross-neutralizing antibodies that may mediate cross-protection. Vaccine 2011;29(11):2011-14. [PMID: 21241731]
Kojic E. M., Cu-Uvin S., Conley L., et al. Human papillomavirus infection and cytologic abnormalities of the anus and cervix among HIV-infected women in the study to understand the natural history of HIV/AIDS in the era of effective therapy (the SUN Study). Sex Transm Dis 2011;38(4):253-59. [PMID: 20966828]
Kojic E. M., Kang M., Cespedes M. S., et al. Immunogenicity and safety of the quadrivalent human papillomavirus vaccine in HIV-1-infected women. Clin Infect Dis 2014;59(1):127-35. [PMID: 24723284]
Kutlubay Z., Engin B., Zara T., et al. Anogenital malignancies and premalignancies: facts and controversies. Clin Dermatol 2013;31(4):362-73. [PMID: 23806153]
Labanca T., Mañero I. Vulvar condylomatosis after sex reassignment surgery in a male-to-female transsexual: complete response to imiquimod cream. Gynecol Oncol Rep 2017;20:75-77. [PMID: 28349118]
Lacey C. J., Woodhall S. C., Wikstrom A., et al. 2012 European guideline for the management of anogenital warts. J Eur Acad Dermatol Venereol 2013;27(3):e263-70. [PMID: 22409368]
Leeds I. L., Fang S. H. Anal cancer and intraepithelial neoplasia screening: A review. World J Gastrointest Surg 2016;8(1):41-51. [PMID: 26843912]
Lichter K., Krause D., Xu J., et al. Adjuvant human papillomavirus vaccine to reduce recurrent cervical dysplasia in unvaccinated women: a systematic review and meta-analysis. Obstet Gynecol 2020;135(5):1070-83. [PMID: 32282601]
Liguori G., Trombetta C., Bucci S., et al. Condylomata acuminata of the neovagina in a HIV-seropositive male-to-female transsexual. Urol Int 2004;73(1):87-88. [PMID: 15263800]
Lillo F. B., Ferrari D., Veglia F., et al. Human papillomavirus infection and associated cervical disease in human immunodeficiency virus-infected women: effect of highly active antiretroviral therapy. J Infect Dis 2001;184(5):547-51. [PMID: 11494160]
Lin C., Franceschi S., Clifford G. M. Human papillomavirus types from infection to cancer in the anus, according to sex and HIV status: a systematic review and meta-analysis. Lancet Infect Dis 2018;18(2):198-206. [PMID: 29158102]
Liu G., Sharma M., Tan N., et al. HIV-positive women have higher risk of human papilloma virus infection, precancerous lesions, and cervical cancer. AIDS 2018;32(6):795-808. [PMID: 29369827]
Lofgren S. M., Tadros T., Herring-Bailey G., et al. Progression and regression of cervical pap test lesions in an urban AIDS clinic in the combined antiretroviral therapy era: a longitudinal, retrospective study. AIDS Res Hum Retroviruses 2015;31(5):508-13. [PMID: 25693769]
Lowy D. R., Schiller J. T. Reducing HPV-associated cancer globally. Cancer Prev Res (Phila) 2012;5(1):18-23. [PMID: 22219162]
Massad L. S., Xie X., Burk R. D., et al. Association of cervical precancer with human papillomavirus types other than 16 among HIV co-infected women. Am J Obstet Gynecol 2016;214(3):354.e1-6. [PMID: 26433170]
Matsuki S., Kusatake K., Hein K. Z., et al. Condylomata acuminata in the neovagina after male-to-female reassignment treated with CO2 laser and imiquimod. Int J STD AIDS 2015;26(7):509-11. [PMID: 24970474]
McKenzie N. D., Kobetz E. N., Hnatyszyn J., et al. Women with HIV are more commonly infected with non-16 and -18 high-risk HPV types. Gynecol Oncol 2010;116(3):572-77. [PMID: 19906410]
Minkoff H., Ahdieh L., Massad L. S., et al. The effect of highly active antiretroviral therapy on cervical cytologic changes associated with oncogenic HPV among HIV-infected women. AIDS 2001;15(16):2157-64. [PMID: 11684935]
Money D. M., Moses E., Blitz S., et al. HIV viral suppression results in higher antibody responses in HIV-positive women vaccinated with the quadrivalent human papillomavirus vaccine. Vaccine 2016;34(40):4799-4806. [PMID: 27544584]
Moscicki A. B., Shiboski S., Broering J., et al. The natural history of human papillomavirus infection as measured by repeated DNA testing in adolescent and young women. J Pediatr 1998;132(2):277-84. [PMID: 9506641]
National Center for Transgender Equality. The report of the 2015 U.S. Transgender Survey. 2016 Dec. https://transequality.org/sites/default/files/docs/usts/USTS-Full-Report-Dec17.pdf [accessed 2022 Oct 17]
NCI(a). Cancer stat facts: cervical cancer. 2022 Oct 27. https://seer.cancer.gov/statfacts/html/cervix.html [accessed 2022 Oct 17]
NCI(b). Oral cavity, oropharyngeal, hypopharyngeal, and laryngeal cancers prevention (PDQ. 2022 Jun 23. https://www.cancer.gov/types/head-and-neck/hp/oral-prevention-pdq [accessed 2022 Oct 17]
Palefsky J. M. Human papillomavirus-associated anal and cervical cancers in HIV-infected individuals: incidence and prevention in the antiretroviral therapy era. Curr Opin HIV AIDS 2017;12(1):26-30. [PMID: 27828801]
Palefsky J. M., Holly E. A., Hogeboom C. J., et al. Virologic, immunologic, and clinical parameters in the incidence and progression of anal squamous intraepithelial lesions in HIV-positive and HIV-negative homosexual men. J Acquir Immune Defic Syndr Hum Retrovirol 1998;17(4):314-19. [PMID: 9525431]
Palefsky(a) J. M., Holly E. A., Ralston M. L., et al. Effect of highly active antiretroviral therapy on the natural history of anal squamous intraepithelial lesions and anal human papillomavirus infection. J Acquir Immune Defic Syndr 2001;28(5):422-28. [PMID: 11744829]
Palefsky(b) J. M., Holly E. A., Ralston M. L., et al. Prevalence and risk factors for anal human papillomavirus infection in human immunodeficiency virus (HIV)-positive and high-risk HIV-negative women. J Infect Dis 2001;183(3):383-91. [PMID: 11133369]
Petrosky E., Bocchini J. A., Hariri S., et al. Use of 9-valent human papillomavirus (HPV) vaccine: updated HPV vaccination recommendations of the Advisory Committee on Immunization Practices. MMWR Morb Mortal Wkly Rep 2015;64(11):300-304. [PMID: 25811679]
Piketty C., Cochand-Priollet B., Lanoy E., et al. Lack of regression of anal squamous intraepithelial lesions despite immune restoration under cART. AIDS 2013;27(3):401-6. [PMID: 23079803]
Poynten I. M., Jin F., Garland S. M., et al. HIV, immune dysfunction, and the natural history of anal high-risk human papillomavirus infection in gay and bisexual men. J Infect Dis 2021;224(2):246-57. [PMID: 33220687]
Richel O., de Vries H. J., van Noesel C. J., et al. Comparison of imiquimod, topical fluorouracil, and electrocautery for the treatment of anal intraepithelial neoplasia in HIV-positive men who have sex with men: an open-label, randomised controlled trial. Lancet Oncol 2013;14(4):346-53. [PMID: 23499546]
Saraiya M., Unger E. R., Thompson T. D., et al. US assessment of HPV types in cancers: implications for current and 9-valent HPV vaccines. J Natl Cancer Inst 2015;107(6):djv086. [PMID: 25925419]
Steinbrook R. The potential of human papillomavirus vaccines. N Engl J Med 2006;354(11):1109-12. [PMID: 16540608]
Stier E. A., Sebring M. C., Mendez A. E., et al. Prevalence of anal human papillomavirus infection and anal HPV-related disorders in women: a systematic review. Am J Obstet Gynecol 2015;213(3):278-309. [PMID: 25797230]
Tyerman Z., Aboulafia D. M. Review of screening guidelines for non-AIDS-defining malignancies: evolving issues in the era of highly active antiretroviral therapy. AIDS Rev 2012;14(1):3-16. [PMID: 22297500]
UCSF. Transgender care & treatment guidelines: creating a safe and welcoming clinic environment. 2016 Jun 17. https://transcare.ucsf.edu/guidelines/clinic-environment [accessed 2022 Oct 17]
van der Sluis W. B., Buncamper M. E., Bouman M. B., et al. Symptomatic HPV-related neovaginal lesions in transgender women: case series and review of literature. Sex Transm Infect 2016;92(7):499-501. [PMID: 27013740]
Wang C. J., Palefsky J. M. HPV-associated anal cancer in the HIV/AIDS patient. Cancer Treat Res 2019;177:183-209. [PMID: 30523625]
Wasef W., Sugunendran H., Alawattegama A. Genital warts in a transsexual. Int J STD AIDS 2005;16(5):388-89. [PMID: 15949073]
Werner R. N., Westfechtel L., Dressler C., et al. Anogenital warts and other HPV-associated anogenital lesions in the HIV-positive patient: a systematic review and meta-analysis of the efficacy and safety of interventions assessed in controlled clinical trials. Sex Transm Infect 2017;93(8):543-50. [PMID: 28637906]
Weyers S., De Sutter P., Hoebeke S., et al. Gynaecological aspects of the treatment and follow-up of transsexual men and women. Facts Views Vis Obgyn 2010;2(1):35-54. [PMID: 25206965]
Wheeler C. M., Castellsagué X., Garland S. M., et al. Cross-protective efficacy of HPV-16/18 AS04-adjuvanted vaccine against cervical infection and precancer caused by non-vaccine oncogenic HPV types: 4-year end-of-study analysis of the randomised, double-blind PATRICIA trial. Lancet Oncol 2012;13(1):100-110. [PMID: 22075170]
Wilkin T. J., Chen H., Cespedes M. S., et al. A randomized, placebo-controlled trial of the quadrivalent human papillomavirus vaccine in human immunodeficiency virus-infected adults aged 27 years or older: AIDS Clinical Trials Group Protocol A5298. Clin Infect Dis 2018;67(9):1339-46. [PMID: 29659751]
Workowski K. A., Bachmann L. H., Chan P.A., et al. Sexually transmitted diseases treatment guidelines, 2021. MMWR Recomm Rep 2021;70(RR-4):1-187. [PMID: 26042815]
Updates, Authorship, and Related Guidelines
| Updates, Authorship, and Related Guidelines | |
| Date of original publication | July 10, 2018 |
| Date of current publication | November 04, 2022 |
| Highlights of changes, additions, and updates in the November 04, 2022 edition |
|
| Intended users | Clinicians in New York State who provide care to individuals with HIV |
| Lead author |
Meera Shah, MD, MPH, MS, AAHIVS |
| Contributing author(s) |
Maria Teresa Timoney, MS, RN, CNM; Jessica M. Atrio, MD, MSc |
| Writing group |
Steven M. Fine, MD, PhD; Rona M. Vail, MD; Joseph P. McGowan, MD, FACP, FIDSA; Samuel T. Merrick, MD; Asa E. Radix, MD, MPH, PhD; Charles J. Gonzalez, MD; Christopher J. Hoffmann, MD, MPH |
| Author and writing group conflict of interest disclosures |
Joseph P. McGowan, MD, FACP, FIDSA: Institutional Pharma grant recipient/support, clinical trial; Gilead |
| Committee | |
| Developer and funder |
New York State Department of Health AIDS Institute (NYSDOH AI) |
| Development process |
See Guideline Development and Recommendation Ratings Scheme, below. |
| Related NYSDOH AI guidelines |
Guidelines
Guidance
Podcast |
Guideline Development and Recommendation Ratings
| Guideline Development: New York State Department of Health AIDS Institute Clinical Guidelines Program | |
| Program manager | Clinical Guidelines Program, Johns Hopkins University School of Medicine, Division of Infectious Diseases. See Program Leadership and Staff. |
| Mission | To produce and disseminate evidence-based, state-of-the-art clinical practice guidelines that establish uniform standards of care for practitioners who provide prevention or treatment of HIV, viral hepatitis, other sexually transmitted infections, and substance use disorders for adults throughout New York State in the wide array of settings in which those services are delivered. |
| Expert committees | The NYSDOH AI Medical Director invites and appoints committees of clinical and public health experts from throughout New York State to ensure that the guidelines are practical, immediately applicable, and meet the needs of care providers and stakeholders in all major regions of New York State, all relevant clinical practice settings, key New York State agencies, and community service organizations. |
| Committee structure |
|
| Disclosure and management of conflicts of interest |
|
| Evidence collection and review |
|
| Recommendation development |
|
| Review and approval process |
|
| External reviews |
|
| Update process |
|
| Recommendation Ratings Scheme | |||
| Strength | Quality of Evidence | ||
| Rating | Definition | Rating | Definition |
| A | Strong | 1 | Based on published results of at least 1 randomized clinical trial with clinical outcomes or validated laboratory endpoints. |
| B | Moderate | * | Based on either a self-evident conclusion; conclusive, published, in vitro data; or well-established practice that cannot be tested because ethics would preclude a clinical trial. |
| C | Optional | 2 | Based on published results of at least 1 well-designed, nonrandomized clinical trial or observational cohort study with long-term clinical outcomes. |
| 2† | Extrapolated from published results of well-designed studies (including nonrandomized clinical trials) conducted in populations other than those specifically addressed by a recommendation. The source(s) of the extrapolated evidence and the rationale for the extrapolation are provided in the guideline text. One example would be results of studies conducted predominantly in a subpopulation (e.g., one gender) that the committee determines to be generalizable to the population under consideration in the guideline. | ||
| 3 | Based on committee expert opinion, with rationale provided in the guideline text. | ||
Last updated on March 25, 2026

